For asymptomatic patients who are ACPA (anti-citrullinated peptide antibody) positive, inflammation detected on power Doppler ultrasound portends for development of RA in the near future.
Grey scale and power Doppler ultrasound activity correlates with joint erosion, which is a predictor for aggressive RA that may likely progress rapidly to joint damage if not optimally treated in timely fashion.
-
OMERACT-EULAR composite PDUS synovitis score
-
Grade 0 (normal joint): no greyscale-detected synovial hyperplasia and no PD signal
-
Grade 1 (minimal synovitis): grade 1 synovial hyperplasia and </= grade 1 PD signal
-
Grade 2 (moderate synovitis): grade 2 synovial hyperplasia and </= grade 2 PD signal; or grade 1 synovial hyperplasia and a grade 2 PD signal
-
Grade 3 (severe synovitis): grade 3 synovial hyperplasia and </= grade 3 PD signal; or grade 1 or 2 synovial hyperplasia and a grade 3 PD signal
-
Synovitis as assessed on ultrasound is a sensitive and early indicator of response to therapy in RA. This is especially important for those on expensive biologics (like Abatacept in this study), so that decisions to switch therapy can be made earlier should the joint inflammation remain unabated.
Also, it overcomes the subjective outcome measure of pain, which may arise from other conditions like Fibromyalgia, and complicate the clinical assessment of RA disease activity.
The 6-million dollar question: would a more stringent remission standard, namely sonographic as compared to the current clinical remission criteria (incorporating physical examination, blood tests, patient’s and physician’s assessment), result in better patient outcomes in terms of pain relief, functional restoration and prevention of radiographic joint damage?
The answer for now is apparently, NO.
Using a sonographic target of deeper remission than is clinically evident did not produce better outcomes (which were pretty good to begin with).
Instead, it led to greater use of expensive biologics in an attempt to induce that deeper remission, in addition to more time and cost consumed in incorporating ultrasound at every clinic visit, thereby increasing overall costs.
A case of diminishing returns?
For now. The TUI group may yet strike back.
The holy grail of remission is histological. We’re currently doing clinical, and we saw from the previous post that that may be enough for now, without having to resort to a sonographic remission target.
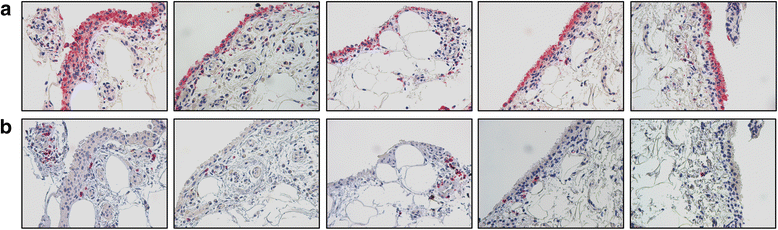
This article demonstrates that remission does follow a continuum, with sonographic remission, especially power Doppler, more closely reflective of minimal histological disease activity.
Does it matter? Maybe not if you’re merely targeting RA disease control to prevent damage progression and disability. However, if you’re hoping for tapering of therapies and even going off treatment, the next 2 articles will show the relevance of seeking a sonographic remission.
The deeper the remission, the more likely you are able to taper down therapy and hopefully even go off all treatment. Ultimate remission is histological, where no (or scant) inflammatory cells remain in the joint synovium.
Short of doing repeated synovial biopsies to gauge histological remission, the power Doppler ultrasound is the closest approximation of this nirvanic state.
Unfortunately, even in sonographic remission, some histological inflammatory disease persists. suggesting that one may never be rid of the disease. Fortunately, with the non-invasive ready accessibility of ultrasound, the patient can be monitored for impending relapse off medication, so as to effectively reinstitute low intensity treatment before the arthritis flares clinically.
This is the clinical proof for targeting deep remission (sonographic) to achieve successful tapering.